SA Task force explores student sexual health
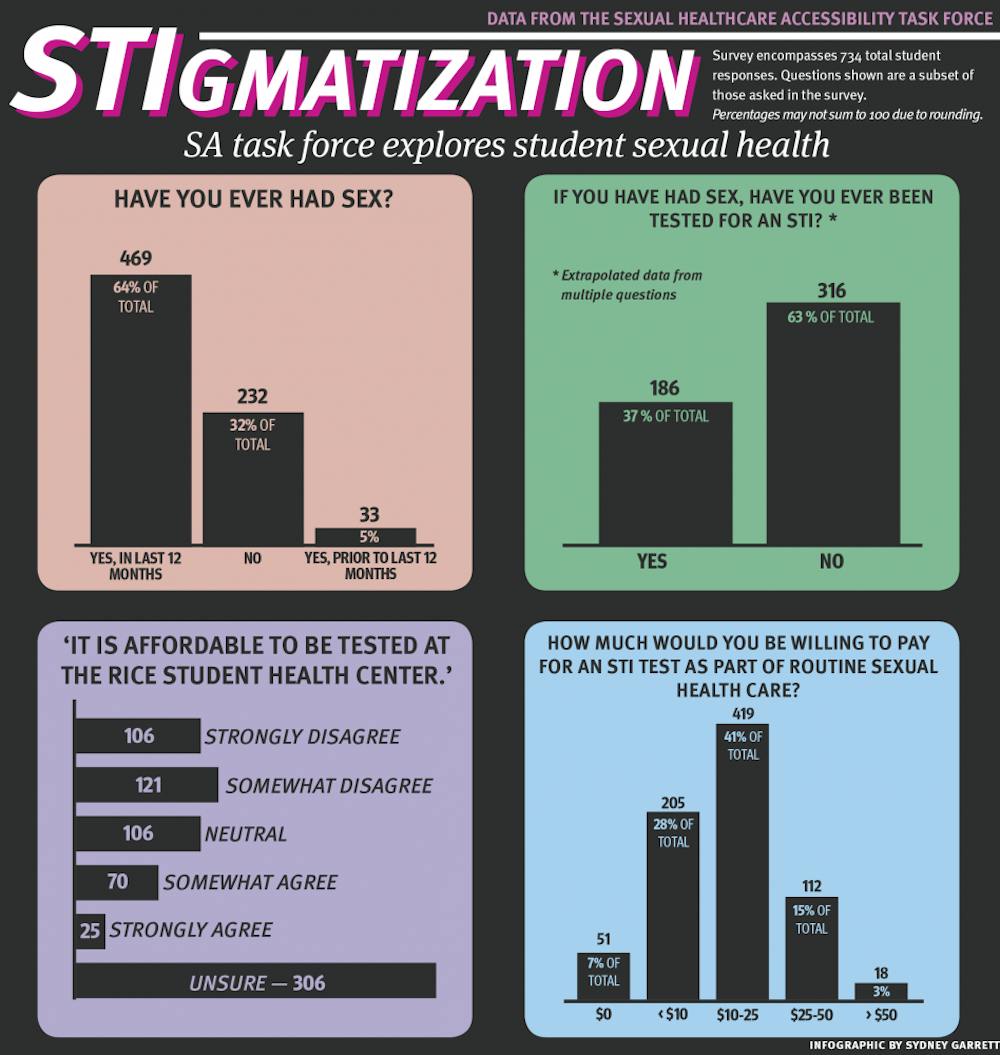
The Student Association Sexual Healthcare Accessibility Task Force has identified a disparity between what students are willing to pay for Sexually Transmitted Infection tests and the prices offered by Health Services from its recent survey on STI testing.
According to director of Student Health Services Dr. Jessica McKelvey, a comprehensive STI test for gonorrhea, chlamydia, HIV and syphilis costs $74. Only 4 percent of the 734 undergraduate respondents were willing to pay this price, while 76 percent of respondents would not pay above $25 for testing.
“That’s just not the price of the health center,” task force co-Chair Blake Coleman said. “If that’s the price that people need to get generally tested, then that should correlate to what the health center’s offering.”
McKelvey said no further reductions to STI testing costs are expected as they have already been reduced.
“We offer substantial discounts on [STI] testing,” McKelvey said. “We were able to negotiate even further reductions this school year and the price for doing all four tests dropped by $20.”
The survey, which was released Jan. 15, asked students a number of questions related to STI testings. According to Coleman, a Brown College freshman and New Student Representative who co-leads the task force with Brown Senator Grace Wickerson, the survey was online for three weeks and received 734 responses. Wickerson said she believes the number of responses received makes it a large sampling of the student body.
Wickerson, a sophomore, said the SA Senate created the task force in November 2017 after Wickerson formed the idea from talking to fellow members of Brown College. The task force consists of 10 students divided into four teams: short-term initiatives, administrative relations, data analysis and peer institution research.
“Our goal as a group is to develop a comprehensive set of actionable items for increasing access to sexual health care at Rice,” Wickerson said. “We plan to do so by investigating why sexual health care is so expensive at Rice and what we can do about it, as well as understanding student opinions on sexual health care to develop plans that meet their needs.”
Coleman said some results from the survey that stood out were the high number of students who are sexually active coupled with the low number of students who have been tested for STIs. A survey question on sexual activity found that 63.9 percent of students reported having oral, vaginal or anal sex in the past 12 months, while 73.2 percent of students reported never having been tested. Over half of sexually active respondents said they had never been tested.
Most students choose to get tested for HIV, syphilis, gonorrhea and chlamydia, according to McKelvey. Individual HIV or syphilis tests fall below $25, while individual tests for gonorrhea or chlamydia cost $46.
McKelvey said that Health Services also offers $195 HPV vaccination shots, for which students under Aetna insurance can be fully reimbursed. According to McKelvey, HPV testing is not recommended for students under 30 years of age as per the US Preventive Services Task Force.
Coleman said compared to other universities, Rice is one of the few that requires students to pay out-of-pocket for STI testing. Coleman said students at Princeton and Columbia Universities are offered free HIV testing, and universities such as Dartmouth and Cornell incorporate testing costs into part of their student health fees.
Coleman also said the large number of students who were unsure about information related to Student Health Services was problematic. The survey found that 41.7 percent of students claimed they were unsure whether it is affordable to get tested at the health center, and 27.2 percent of respondents did not know the health center provides testing.
“That means the health center is not doing enough publicity-wise of getting out that they offer testing,” Coleman said.
Coleman said updating the health center’s webpage on STI testing is one way to improve publicity of the testing services offered. The current page has a total of four sentences and 40 words.

“It’s not very descriptive at all, and if you compare it to other institutions, they have a whole page on their website or something like that dedicated to how the sexual tests work at that campus and what the process is with that,” Coleman said.
Coleman said that the task force is attempting to find out why Rice students are not covered in the same way as students elsewhere despite having the same insurance plan.
“A big thing with this is that we’re sort of confused why Rice requires students to get on the Aetna Insurance plan yet it still doesn’t cover the STI testing, whereas other universities also use Aetna but it does cover the STI testing at those universities,” Coleman said.
McKelvey said testing at Health Services is not covered because the office is not in any insurance company’s network and does not have a billing department.
“Students may use their own insurance for free [STI] testing at outside providers,” McKelvey said.
“Most insurances, including Aetna Student Health, include preventive STD testing as per the U.S. Preventive Services Task Force recommendations. We are not insurance preferred providers as the cost to do this would be astronomical, so the insurance bill does need to be outside of Rice.”
McKelvey also said that in February of 2014, the health center collaborated with a Rice Health Adviser from Wiess College to temporarily offer free HIV testing. The student, who McKelvey did not name, advertised the event himself, and Health Services conducted 52 free tests in one week.
“He obtained a grant through the Dr. Bill [Wilson Student Initiative] Grant at Wiess College to pay for student testing during Valentine’s week,” McKelvey said.”It was a great project and we are glad to collaborate with any student projects in the future.”
Coleman said the survey results will provide a basis to start the conversation about increased sexual healthcare accessibility.
“Honestly, the survey results are almost speaking for themselves in what we really need to do, so we hope with this survey we can reach out to the administration more, just start the discourse,” Coleman said. “Start pushing for the change that we need.”
More from The Rice Thresher

Rice Students for Justice in Palestine declares ‘liberated zone’ on campus
As student protests erupt across the country, Rice Students for Justice in Palestine launched a “liberated zone” on Rice campus, announced a two-day series of events and started construction on an “apartheid wall.”

Jeremy Zucker headlines second-ever Moody X-Fest
Jeremy Zucker headlined Rice’s second annual Moody X-Fest in Founder’s Court on April 19. In advance of Zucker’s set, student groups like Basmati Beats, Rice Philharmonic and BASYK performed. The festival also offered complimentary merchandise and food from Dripped Birra, Cane’s and Oh my Gogi.

Jones wins men’s and women’s Beer Bike races, GSA snags alumni
Jones College won both the women’s and men’s Beer Bike 2024 races, while the Graduate Student Association claimed the alumni team win. Hanszen College bike teams were the runner-up in the alumni and men’s races, while Brown College was the runner-up in the women’s race. Martel and McMurtry Colleges did not bike in the alumni race, according to the Rice Program Council’s final report, and the GSA was disqualified from the men’s race for accidentally sending out two bikers simultaneously.

Please note All comments are eligible for publication by The Rice Thresher.